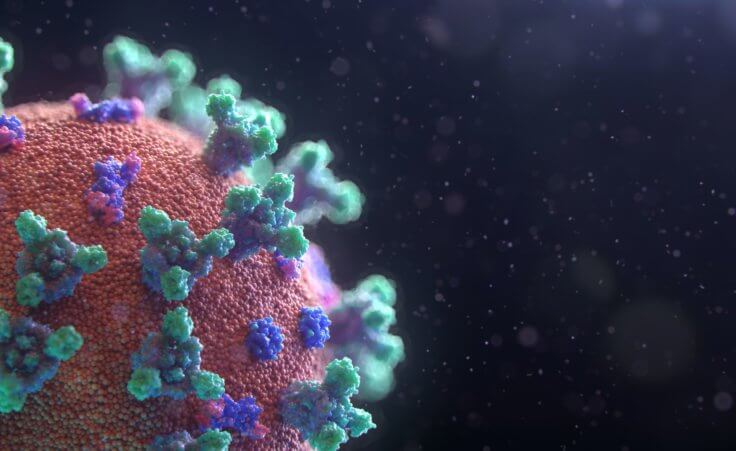
Get ready for your next doctor’s visit to take longer than last time. New regulations are set to take effect October 1 that will drastically change the entire healthcare industry. The shift is how doctors code ailments and receive reimbursement from insurance companies. For decades the U.S. has used the ICD-9 standard of coding, which has approximately 14,000 diagnostic codes, but come October 1 that number will expand to over 70,000 codes as the U.S. implements ICD-10.
In the old system there were about 16 ways to code a broken femur, for instance, while in the new system that number will skyrocket to 750. The American Medical Association has long opposed the move to ICD-10, arguing that it will cause a nightmare of backlogged payments that will wreak havoc as doctors and their assistants attempt to learn the vast new codes. While proponents for the move cite that ICD-10 is already the worldwide standard of codes, in reality each country has specific alterations it makes, lessening the power of the “we need to update because the rest of the world already has” argument.
While it is true that ICD-10 is a worldwide standard, the U.S. is already far behind, and ICD-11 is only a few years away (2017-18). The medical coding overhaul will bring with it challenges, but will bring positive updates as well. The difficulty is assessing how much the potential gains will be mitigated by the troubles they cause. The law of unintended consequences proves that despite the best planning and preparation, (which are debatable at this point) unseen challenges always emerge when rolling out a new system.
From a leadership standpoint, one could argue the merits of the move itself, but that is not the goal here. Let’s look instead at how this change represents our culture’s overall shift to one that unflinchingly trusts in technocratic principles.
James Kalb, in the September issue of First Things, describes our contemporary society as technocratic in that it “recognizes no transcendent authority above it, no history behind it expect the history of its own coming into being, and no nature of things beneath it that cannot be transformed technologically into what we choose.” We assume that every technological innovation is good because we have thrown off the shackles of out-dated, out-moded ways of thinking about the world.
The key concept underlying this shift to a technocratic society is that it has led to a “continuing reconfiguration of social life, through the replacement of traditional precepts by technological methods keyed to utility and equality.” We assume that updating our healthcare coding will lead to greater utility by helping more people and providing more precision in information sharing. It’s the same belief that underlies many in our educational system who believe that if we can just modernize and codify and streamline our teaching, everything will be better.
Blind belief in technology is the air our culture breathes, but its properties are tinged with dangerous, toxic consequences. One of the great concerns that should come to the fore anytime we adopt new, more detailed standards, is how much people can actually use them in practice. We’ve all seen how the stock market has been taken over by algorithmic trading that leads many to wonder how much any financial “expert” actually knows about the market. Similarly, one can envision doctor’s offices getting lost in the minutiae of ICD-10.
Technology creates greater complexity, and we are notoriously awful at handling complexity as humans. The leadership takeway from this exploration into ICD-10 and its technocratic underpinnings is that leaders need to understand the human component behind all change endeavors.
Whether or not a change should be undertaken is another question, but when that change is decided upon, leaders must think through how the change will impact real people on the ground, at every level of the organization. This takes time and thoughtful debate. Scripture constantly speaks of and illustrates the principle that wise counsel is essential to good leadership (see Proverbs 11:14; 15:22; 20:18; Luke 14:31). We would ignore this principle at our own, and our organizations, peril.